Welcome to our comprehensive guide on fatty liver disease! Whether you’re an adult concerned about your own health or a caregiver looking out for your loved one, this post is tailored to provide you with all the vital information you need. Fatty liver disease is a growing health issue that affects millions worldwide, and understanding its causes, symptoms, and treatment is crucial for maintaining a healthy liver. In this post, we’ve compiled 60 of the most reliable and relevant medical questions and answers to cover every aspect of this condition. So grab a cup of tea, sit back, and get ready to dive into the world of fatty liver disease!
In the Quest for Knowledge: 60 Expert Answers to Your Fatty Liver Disease Questions
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
⚠️ 👀A Supplemental Section of 5 Questions and Answers About the possible use of the Prescription Medication, Ozempic (Semaglutide) for the treatment of FLD has been added to the bottom of the Main Article just after the Answer to Question 60, Before the Additional References Section.
The 60 Fatty Liver Disease Questions:
1. What is Fatty Liver Disease, and what are its causes?
2. Can Fatty Liver Disease be reversed or cured?
3. How does Fatty Liver Disease affect overall liver function and health?
4. What are the symptoms of Fatty Liver Disease?
5. Are there any specific risk factors associated with the development of Fatty Liver Disease?
6. How is Fatty Liver Disease diagnosed and monitored?
7. What lifestyle changes can help prevent or manage Fatty Liver Disease?
8. What dietary recommendations should individuals with Fatty Liver Disease follow?
9. Are there any specific foods or supplements that can improve liver health in Fatty Liver Disease?
10. What is the connection between Fatty Liver Disease and obesity?
11. Are there any medications available for treating Fatty Liver Disease?
12. How can excessive alcohol consumption contribute to Fatty Liver Disease?
13. Can Fatty Liver Disease lead to liver cirrhosis or liver cancer?
14. Can Fatty Liver Disease affect people who are not overweight?
15. Are there any potential complications associated with Fatty Liver Disease?
16. How does Fatty Liver Disease impact overall cardiovascular health?
17. Can Fatty Liver Disease cause or worsen diabetes and insulin resistance?
18. Is it possible to reverse Fatty Liver Disease through exercise alone?
19. What are the long-term consequences of untreated Fatty Liver Disease?
20. Are there any natural remedies or alternative treatments for Fatty Liver Disease?
21. How does Fatty Liver Disease affect the absorption and processing of nutrients?
22. Can stress and mental health issues contribute to the development or progression of Fatty Liver Disease?
23. Is there a genetic component to Fatty Liver Disease?
24. Can Fatty Liver Disease be prevented in individuals with a family history of the condition?
25. What effects do certain medications have on Fatty Liver Disease?
26. Can Fatty Liver Disease lead to liver failure?
27. How often should liver function tests be conducted in individuals with Fatty Liver Disease?
28. Can Fatty Liver Disease be managed without medical intervention?
29. What role does inflammation play in the development and progression of Fatty Liver Disease?
30. Are there any specific exercises or physical activities that can help improve liver health in Fatty Liver Disease?
31. Can Fatty Liver Disease be diagnosed without performing a liver biopsy?
32. How does Fatty Liver Disease affect cholesterol levels in the body?
33. Can Fatty Liver Disease affect hormone balance and reproductive health?
34. Are there any potential drug interactions to be aware of for individuals with Fatty Liver Disease?
35. What impact does Fatty Liver Disease have on the immune system?
36. Can Fatty Liver Disease cause or worsen gallbladder problems?
37. Are there any gender-specific considerations when it comes to Fatty Liver Disease?
38. Can Fatty Liver Disease be managed through intermittent fasting or specific eating schedules?
39. How does Fatty Liver Disease relate to other liver diseases, such as hepatitis?
40. Can Fatty Liver Disease affect cognitive function and brain health?
41. What role do antioxidants play in managing Fatty Liver Disease?
42. Can Fatty Liver Disease be a result of certain viral infections?
43. How does Fatty Liver Disease impact the body’s ability to detoxify harmful substances?
44. Can Fatty Liver Disease cause digestive issues or gastrointestinal problems?
45. Does Fatty Liver Disease increase the risk of developing certain types of cancer?
46. How does Fatty Liver Disease affect the body’s ability to metabolize carbohydrates and sugars?
47. Can Fatty Liver Disease cause or worsen sleep disorders?
48. How does Fatty Liver Disease impact the absorption and utilization of vitamins and minerals?
49. Are there any support groups or resources available for individuals with Fatty Liver Disease?
50. Can certain herbal supplements help improve liver health in Fatty Liver Disease?
51. How long does it typically take for Fatty Liver Disease to progress from mild to severe stages?
52. Can Fatty Liver Disease be managed in individuals with limited mobility or physical disabilities?
53. How does Fatty Liver Disease affect the body’s ability to process medications?
54. Can Fatty Liver Disease cause nutritional deficiencies?
55. What role does gut health play in the development and management of Fatty Liver Disease?
56. Can Fatty Liver Disease lead to an increased risk of heart attack or stroke?
57. How does Fatty Liver Disease affect the body’s metabolism and energy levels?
58. Can Fatty Liver Disease affect a person’s mental health and emotional well-being?
59. What impact does Fatty Liver Disease have on overall life expectancy?
60. Are there any specific precautions or considerations for seniors or individuals with physical or mental dependencies who have Fatty Liver Disease?
💊While I do cite reputable sources, I am not a medical professional. Please use professional medical advice when making any health-related decisions.
1. What is Fatty Liver Disease, and what are its causes?
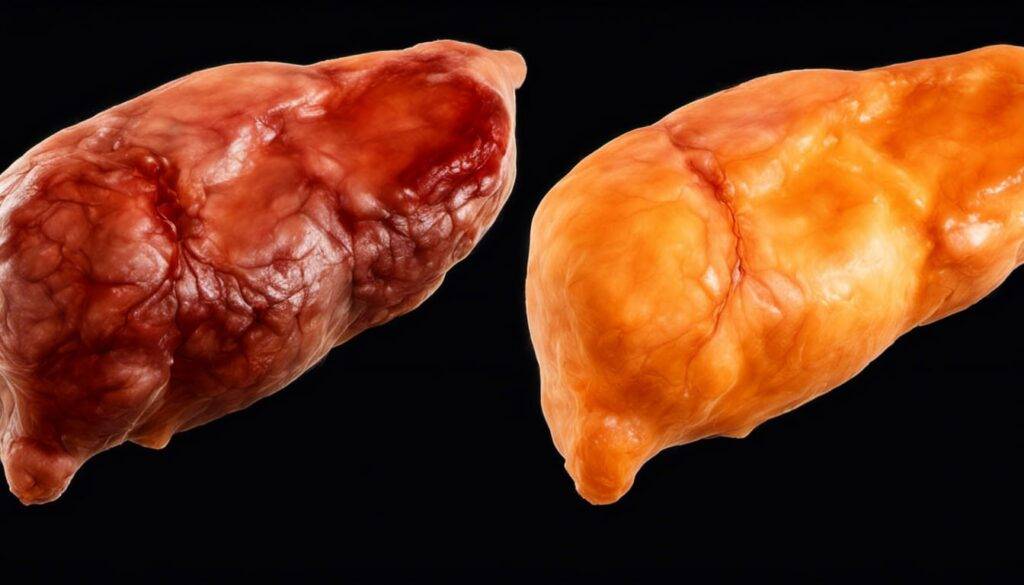
Fatty Liver Disease, also known as hepatic steatosis, is a condition characterized by the accumulation of excess fat in the liver. This build-up can impair liver function and lead to various health problems. The causes of Fatty Liver Disease can be broadly categorized into two types: alcoholic and nonalcoholic. Alcoholic Fatty Liver Disease is caused by excessive alcohol consumption, which can lead to fat deposition in the liver. Nonalcoholic Fatty Liver Disease (NAFLD) can stem from factors such as obesity, insulin resistance, high blood sugar, high cholesterol levels, and metabolic syndrome. It is important to address these underlying causes to effectively manage and prevent the progression of the disease.
Bonus Fact: Fatty Liver Disease is considered to be one of the most common liver diseases worldwide, affecting both adults and children.
Source:
Title: “Nonalcoholic Fatty Liver Disease“
URL: https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
2. Can Fatty Liver Disease be reversed or cured?
Yes, Fatty Liver Disease can be reversed, but the success of treatment depends on the underlying causes and stage of the disease. For alcoholic Fatty Liver Disease, the primary recommendation is to stop consuming alcohol completely. This can help alleviate fat accumulation and allow the liver to heal over time. In nonalcoholic Fatty Liver Disease, lifestyle modifications play an essential role in managing the disease. These modifications include adopting a healthy diet, engaging in regular physical activity, achieving and maintaining a healthy weight, and controlling conditions such as diabetes and high cholesterol. By addressing these factors, it is possible to improve liver health, reduce fat accumulation, and reverse the effects of the disease.
Bonus Fact: Fatty Liver Disease is often asymptomatic, meaning it may not cause noticeable symptoms in the early stages. Regular liver function evaluations and screenings are crucial to detect and manage the disease effectively.
Source:
Title: “Reverse your fatty liver: The comprehensive guide to a healthy liver“
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3350655/
3. How does Fatty Liver Disease affect overall liver function and health?
Fatty Liver Disease can have a significant impact on overall liver function and health. The excessive accumulation of fat in the liver can lead to inflammation and damage the liver cells, impairing their ability to function normally. As the disease progresses, it can cause a condition called fibrosis, where the liver develops scar tissue. If left untreated, this scar tissue can progress to a more severe condition known as cirrhosis, which leads to loss of liver function. Furthermore, Fatty Liver Disease increases the risk of developing liver cancer. Thus, it is important to address the underlying causes and manage the disease promptly to preserve liver function and overall health.
Bonus Fact: Fatty Liver Disease is closely linked to insulin resistance and is considered an early sign of metabolic syndrome.
Source:
Title: “Nonalcoholic Fatty Liver Disease (NAFLD) – Symptoms and Causes“
URL: https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567
4. What are the symptoms of Fatty Liver Disease?
Fatty Liver Disease may not cause noticeable symptoms in its early stages. However, as the disease progresses, some common symptoms may manifest. These include fatigue, weakness, abdominal discomfort or pain in the upper right portion, enlarged liver (hepatomegaly), and yellowing of the skin and eyes (jaundice) in severe cases. It is important to note that these symptoms can also be associated with other liver diseases. Therefore, accurate diagnosis and evaluation through medical consultations and imaging tests are crucial to determine the presence and severity of Fatty Liver Disease.
Bonus Fact: Fatty Liver Disease is closely linked to lifestyle factors such as sedentary behavior and unhealthy dietary habits.
Source:
Title: “Fatty Liver Disease: Overview and More“
URL: https://www.healthline.com/health/fatty-liver
5. Are there any specific risk factors associated with the development of Fatty Liver Disease?
Yes, several specific risk factors are associated with the development of Fatty Liver Disease. In the case of nonalcoholic Fatty Liver Disease (NAFLD), obesity, particularly abdominal obesity, is a significant risk factor. Other risk factors include insulin resistance or Type2 diabetes, high blood pressure, high cholesterol levels, metabolic syndrome, and an unhealthy diet high in processed foods, sugars, and saturated fats. Genetic factors, rapid weight loss, certain medications, and viral hepatitis can also contribute to the development of Fatty Liver Disease.
Bonus Fact: Fatty Liver Disease is more prevalent in individuals with certain medical conditions, such as polycystic ovary syndrome (PCOS) and sleep apnea.
Source:
Title: “Non-Alcoholic Fatty Liver Disease (NAFLD)“
URL: https://www.liverfoundation.org/for-patients/about-the-liver/diseases-of-the-liver/non-alcoholic-fatty-liver-disease/
6. How is Fatty Liver Disease diagnosed and monitored?
In order to diagnose Fatty Liver Disease, a healthcare provider will typically start by reviewing the patient’s medical history, conducting a physical examination, and ordering blood tests. Blood tests, such as liver function tests and imaging studies like ultrasound or MRI, can help in the evaluation and diagnosis of Fatty Liver Disease.
To monitor Fatty Liver Disease, healthcare providers may recommend regular blood tests to assess liver function and to monitor levels of liver enzymes and markers of liver inflammation. Imaging studies, such as ultrasound or MRI, can also be repeated periodically to assess the progression or improvement of the disease.
Bonus Fact: One non-invasive diagnostic tool used to assess the severity of Fatty Liver Disease is a transient elastography or FibroScan. It uses ultrasound waves to measure liver stiffness, which can indicate the degree of fibrosis or scarring in the liver.
Source:
Mayo Clinic. (2021). Nonalcoholic fatty liver disease. https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/diagnosis-treatment/drc-20354573
7. What lifestyle changes can help prevent or manage Fatty Liver Disease?
Lifestyle changes play a crucial role in both preventing and managing Fatty Liver Disease. Here are some recommendations:
1. Maintain a healthy weight: Losing excess weight can reduce the accumulation of fat in the liver. Gradual weight loss, achieved through a balanced diet and regular exercise, can be beneficial.
2. Engage in regular physical activity: Exercise improves insulin sensitivity and helps burn stored fat, including in the liver. Aim for at least 150 minutes of moderate-intensity aerobic exercise per week, or as advised by your healthcare provider.
3. Eat a balanced diet: Choose a diet rich in fruits, vegetables, whole grains, and lean proteins. Limit your intake of saturated and trans fats, refined carbohydrates, sugary foods, and beverages.
4. Limit alcohol consumption: Excessive alcohol consumption can worsen liver damage. If you have Fatty Liver Disease, it’s important to avoid or minimize alcohol intake.
5. Manage medical conditions: Control underlying conditions like diabetes, high cholesterol, and hypertension, as they can contribute to Fatty Liver Disease.
Bonus Fact: Some studies suggest that regular consumption of coffee, specifically caffeinated coffee, may be associated with a reduced risk of developing liver fibrosis or cirrhosis in individuals with Fatty Liver Disease.
Source:
National Institute of Diabetes and Digestive and Kidney Diseases. (2019). Nonalcoholic Fatty Liver Disease (NAFLD) & NASH. https://www.niddk.nih.gov/health-information/liver-disease/nafld-nash/definition-facts
8. What dietary recommendations should individuals with Fatty Liver Disease follow?
Individuals with Fatty Liver Disease can benefit from following a healthy, balanced diet. Here are some dietary recommendations:
1. Choose complex carbohydrates: Opt for whole grains, legumes, and vegetables, which provide fiber and essential nutrients. Avoid or limit refined carbohydrates and sugary foods.
2. Increase intake of fruits and vegetables: These are rich in antioxidants and fiber, which can help reduce inflammation and protect the liver.
3. Consume lean proteins: Include sources such as poultry, fish, tofu, legumes, and low-fat dairy products. Avoid or limit red meat, processed meats, and full-fat dairy.
4. Limit saturated and trans fats: Reduce consumption of fried foods, fatty meats, full-fat dairy products, and commercially baked goods. Instead, opt for healthier fats like avocados, nuts, and olive oil.
5. Stay hydrated: Drink an adequate amount of water daily to support overall health and liver function.
Bonus Fact: Turmeric, a spice commonly used in Indian cuisine, contains an active compound called curcumin, which has shown some potential benefits for liver health, including reducing inflammation and liver fat accumulation in individuals with Fatty Liver Disease.
Source:
American Liver Foundation. (2021). Fatty Liver Disease. https://liverfoundation.org/for-patients/about-the-liver/diseases-of-the-liver/fatty-liver/
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
9. Are there any specific foods or supplements that can improve liver health in Fatty Liver Disease?
Certain foods and supplements have been studied for their potential benefits in improving liver health in Fatty Liver Disease. Here are some examples:
1. Coffee: Regular coffee consumption has been associated with a lower risk of liver fibrosis and cirrhosis progression in individuals with liver disease.
2. Green tea: The catechins and antioxidants found in green tea may have protective effects on the liver and help reduce liver fat accumulation.
3. Omega-3 fatty acids: Found in fatty fish like salmon, trout, and sardines, omega-3 fatty acids have been shown to have anti-inflammatory properties and may help improve liver health.
4. Milk thistle: The active ingredient in milk thistle, called silymarin, is a potent antioxidant that may help protect liver cells from damage. However, more research is needed to fully understand its effectiveness in Fatty Liver Disease.
5. Vitamin E: Some studies suggest that vitamin E supplementation may help improve liver enzyme levels and reduce inflammation in Fatty Liver Disease. However, it’s essential to consult with a healthcare provider before starting any supplements.
Bonus Fact: Beetroot juice has shown potential in reducing liver fat and improving liver enzyme levels in individuals with Fatty Liver Disease. Its high content of nitrates and antioxidants may have beneficial effects on liver health.
Source:
WebMD. (2021). Nonalcoholic Fatty Liver Disease (NAFLD) – Treatment and Home Remedies. https://www.webmd.com/digestive-disorders/nonalcoholic-fatty-liver-disease-treatment#1
10. What is the connection between Fatty Liver Disease and obesity?
Obesity is closely linked to the development and progression of Fatty Liver Disease. Excess body weight, particularly abdominal obesity, increases the risk of developing Fatty Liver Disease.
Adipose (fat) tissue in individuals with obesity releases fatty acids into the bloodstream, which are taken up by the liver and converted into fat, leading to the accumulation of fat in the liver. This process, called lipogenesis, contributes to the development of Fatty Liver Disease.
Furthermore, obesity is often associated with other conditions that can promote liver damage, such as insulin resistance, type 2 diabetes, and high cholesterol levels. These metabolic disturbances contribute to inflammation and oxidative stress in the liver, exacerbating Fatty Liver Disease.
Bonus Fact: The prevalence of Fatty Liver Disease is estimated to be around 80-90 % in individuals with obesity and type 2 diabetes.
Source:
World Journal of Gastroenterology. (2017). The epidemiology of nonalcoholic fatty liver disease: A global perspective. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5636208/
11. Are there any medications available for treating Fatty Liver Disease?
Yes, there are medications available for treating Fatty Liver Disease. One such medication is called pioglitazone, which belongs to a class of drugs called thiazolidinediones. Pioglitazone helps to improve insulin sensitivity and reduce fatty deposits in the liver. It has been shown to effectively treat nonalcoholic fatty liver disease (NAFLD) in some cases. Another medication called obeticholic acid is approved for the treatment of primary biliary cholangitis (PBC), which is a type of liver disease that can lead to liver damage. While not specifically approved for Fatty Liver Disease, there is some evidence suggesting it may also be beneficial for NAFLD patients. It is important to note that medication should always be prescribed and monitored by a healthcare professional.
Bonus Fact: Fatty Liver Disease is becoming increasingly common and is estimated to affect around 25% of the global population.
Source: National Institute of Diabetes and Digestive and Kidney Diseases https://www.niddk.nih.gov/health-information/liver-disease/nafld-nash/treatment
12. How can excessive alcohol consumption contribute to Fatty Liver Disease?
Excessive alcohol consumption can contribute to Fatty Liver Disease, specifically a condition called alcoholic fatty liver disease (AFLD). When alcohol is consumed in excess, the liver metabolizes it to break it down. However, the liver can only process a certain amount of alcohol at a time. When alcohol consumption exceeds the liver’s capacity, the excess alcohol gets converted into fat, leading to the accumulation of fatty deposits in the liver. Over time, this can progress to inflammation and liver damage.
Bonus Fact: AFLD can occur even in individuals who do not consume alcohol regularly but engage in episodic binge drinking.
Source: American Liver Foundation https://liverfoundation.org/for-patients/about-the-liver/diseases-of-the-liver/fatty-liver/
13. Can Fatty Liver Disease lead to liver cirrhosis or liver cancer?
Yes, Fatty Liver Disease can potentially lead to liver cirrhosis and liver cancer. In the case of nonalcoholic fatty liver disease (NAFLD), if left untreated, it can progress to a more severe form called nonalcoholic steatohepatitis (NASH). NASH is characterized by inflammation and liver cell damage. Over time, this inflammation can cause scar tissue to build up, leading to liver cirrhosis. Cirrhosis is a late-stage liver disease that can cause irreversible liver damage. Additionally, individuals with NAFLD/NASH have an increased risk of developing liver cancer, especially if they already have cirrhosis.
Bonus Fact: Liver cancer is one of the leading causes of cancer-related deaths worldwide.
Source: World Journal of Gastroenterology
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6164787/
14. Can Fatty Liver Disease affect people who are not overweight?
Yes, Fatty Liver Disease can affect people who are not overweight. While obesity is a common risk factor for nonalcoholic fatty liver disease (NAFLD), it is not the only one. Other factors that can contribute to NAFLD include insulin resistance, type 2 diabetes, high cholesterol, and metabolic syndrome. These conditions can be present in individuals who are not necessarily overweight or obese. In fact, there is a subtype of NAFLD called lean NAFLD, which primarily affects individuals with normal body weight. It is important to address these underlying conditions to manage and prevent the progression of Fatty Liver Disease.
Bonus Fact: NAFLD is known as a silent disease because it often has no symptoms until it reaches more advanced stages.
Source: Mayo Clinic https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567
15. Are there any potential complications associated with Fatty Liver Disease?
Yes, there are potential complications associated with Fatty Liver Disease. NAFLD can progress to nonalcoholic steatohepatitis (NASH), which can cause liver inflammation and lead to liver fibrosis, cirrhosis, and liver failure. Cirrhosis, in turn, can result in complications such as portal hypertension (increased pressure in the liver), ascites (accumulation of fluid in the abdomen), hepatic encephalopathy (brain dysfunction), and esophageal varices (enlarged veins in the esophagus that can bleed). Additionally, individuals with Fatty Liver Disease are at a higher risk of developing cardiovascular disease, type 2 diabetes, and metabolic syndrome, which further increase the chances of complications.
Bonus Fact: Fatty Liver Disease has become a leading cause of liver transplantation worldwide.
Source: Cleveland Clinic https://my.clevelandclinic.org/health/diseases/21239-nafld-non-alcoholic-fatty-liver-disease
16. How does Fatty Liver Disease impact overall cardiovascular health?
Fatty Liver Disease can have a significant impact on cardiovascular health. The excess fat accumulation in the liver can lead to inflammation and the release of harmful substances into the bloodstream. This can increase the risk of developing conditions such as atherosclerosis (hardening of the arteries), high blood pressure, and heart disease. Additionally, Fatty Liver Disease is closely associated with metabolic syndrome, a cluster of conditions that includes obesity, high cholesterol, high blood pressure, and insulin resistance, all of which further contribute to cardiovascular risk.
Bonus Fact: Individuals with non-alcoholic fatty liver disease (NAFLD) have been found to have a 64% increased risk of cardiovascular disease, compared to those without NAFLD.
Source:
Title: Increased risk of cardiovascular disease in NASH
URL: https://pubmed.ncbi.nlm.nih.gov/23091815/
17. Can Fatty Liver Disease cause or worsen diabetes and insulin resistance?
Yes, Fatty Liver Disease can cause and worsen diabetes and insulin resistance. The excess fat in the liver interferes with insulin’s ability to regulate blood glucose levels effectively. This leads to insulin resistance, where the body becomes less responsive to insulin. As a result, the pancreas produces more insulin to compensate, eventually leading to elevated blood sugar levels and the development of type 2 diabetes. Furthermore, insulin resistance can further contribute to the accumulation of fat in the liver, creating a vicious cycle.
Bonus Fact: Non-alcoholic fatty liver disease (NAFLD) is considered a hepatic manifestation of metabolic syndrome, which includes insulin resistance and type 2 diabetes.
Source:
Title: Liver diseases in the cardiometabolic syndrome. Expert Rev Gastroenterol Hepatol.
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4422781/
18. Is it possible to reverse Fatty Liver Disease through exercise alone?
Exercise, particularly aerobic exercise and resistance training, can be beneficial in reversing Fatty Liver Disease. Regular physical activity helps to reduce excess body weight and improves insulin sensitivity, which is crucial for managing and reversing liver fat accumulation. Exercise also stimulates the production of enzymes that promote fat metabolism, thus aiding in the reduction of liver fat content. However, it is important to note that a comprehensive approach including modifications in diet and lifestyle is generally more effective in reversing Fatty Liver Disease.
Bonus Fact: Studies have shown that a combination of exercise and dietary changes leads to more significant improvements in liver fat content compared to exercise alone.
Source:
Title: Exercise reduces liver lipids and visceral adiposity in patients with nonalcoholic steatohepatitis (NASH).
URL: https://pubmed.ncbi.nlm.nih.gov/21292918/
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
19. What are the long-term consequences of untreated Fatty Liver Disease?
Untreated Fatty Liver Disease can have severe long-term consequences. It can progress to more advanced stages, such as non-alcoholic steatohepatitis (NASH), liver fibrosis, cirrhosis, and even liver cancer. NASH involves inflammation and damage to the liver cells, which can lead to scarring and fibrosis. Over time, the accumulation of scar tissue can disrupt liver function and eventually progress to cirrhosis, which is irreversible. Cirrhosis increases the risk of liver failure and liver cancer (hepatocellular carcinoma), which have poor prognosis and can be life-threatening.
Bonus Fact: Fatty Liver Disease has become one of the leading causes of hepatocellular carcinoma, the most common type of liver cancer.
Source:
Title: Non-alcoholic fatty liver disease and hepatocellular carcinoma: a review.
URL: https://pubmed.ncbi.nlm.nih.gov/24786463/
20. Are there any natural remedies or alternative treatments for Fatty Liver Disease?
While maintaining a healthy lifestyle, including a balanced diet and regular exercise, is the primary approach for managing Fatty Liver Disease, there are some natural remedies and alternative treatments that may provide additional benefits. Certain herbal supplements, such as milk thistle, may help protect and support the liver’s function. Other natural remedies include consuming green tea, increasing intake of omega-3 fatty acids, and incorporating spices like turmeric and cinnamon, which have anti-inflammatory properties. However, it is crucial to consult with a healthcare professional before starting any natural remedies, as they may interact with medications or have varying efficacy.
Bonus Fact: Milk thistle extract, derived from a flowering herb, has been traditionally used as a liver tonic and is being explored for its potential benefits in liver diseases.
Source:
Title: Milk thistle for alcoholic and/or hepatitis B or C liver diseases–a systematic cochrane hepato-biliary group review with meta-analyses of randomized clinical trials.
URL: https://pubmed.ncbi.nlm.nih.gov/19787800/
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
21. How does Fatty Liver Disease affect the absorption and processing of nutrients?
Fatty Liver Disease, specifically nonalcoholic fatty liver disease (NAFLD), can impede the absorption and processing of nutrients in several ways. Firstly, the buildup of fat in liver cells can cause inflammation and damage to the liver, leading to a decrease in the production of bile. Bile plays a crucial role in the digestion and absorption of fats, so its reduced production can hinder the breakdown and utilization of dietary fats.
Furthermore, Fatty Liver Disease can disrupt the normal functioning of the liver, impairing its ability to synthesize essential proteins, such as albumin and clotting factors. These proteins are vital for the transport of nutrients, hormones, and vitamins throughout the body. Consequently, impaired protein synthesis can affect the absorption and delivery of nutrients to various organs and tissues.
Moreover, Fatty Liver Disease can lead to insulin resistance, a metabolic condition where cells become less responsive to insulin. Insulin is responsible for regulating glucose metabolism and promoting the uptake of glucose into cells. With insulin resistance, nutrient absorption, particularly glucose, becomes compromised, potentially leading to elevated blood sugar levels and further metabolic disturbances.
Bonus Fact: Fatty Liver Disease is commonly associated with obesity, type 2 diabetes, and high cholesterol levels. However, it can also affect individuals who are lean and metabolically healthy, known as non-obese NAFLD.
Source:
Title: Nonalcoholic Fatty Liver Disease (NAFLD)
22. Can stress and mental health issues contribute to the development or progression of Fatty Liver Disease?
Yes, stress and mental health issues can contribute to the development and progression of Fatty Liver Disease. Stress triggers the release of stress hormones, such as cortisol, which can lead to metabolic changes in the body. Elevated cortisol levels have been associated with insulin resistance and increased fat storage in the liver.
Moreover, individuals experiencing high levels of chronic stress may adopt unhealthy coping mechanisms, such as overeating or excessive alcohol consumption. These behaviors can contribute to weight gain, obesity, and the development of fatty liver.
Mental health issues, such as depression and anxiety, often coexist with Fatty Liver Disease. Studies indicate that depression can impair self-care behaviors, leading to unhealthy eating habits, physical inactivity, and poor medication adherence. These lifestyle factors can worsen the progression of Fatty Liver Disease.
Furthermore, mental health issues can disrupt the hypothalamic–pituitary–adrenal (HPA) axis, a key system controlling stress responses and hormone regulation. Dysregulation of the HPA axis may promote inflammation, which is a contributing factor in the development of liver damage and progression of Fatty Liver Disease.
Bonus Fact: Stress management techniques, such as mindfulness meditation and regular exercise, have shown promising results in reducing liver fat and improving liver health in individuals with Fatty Liver Disease.
Source:
Title: The relationship between stress and NAFLD: From basic science to clinical evidence
23. Is there a genetic component to Fatty Liver Disease?
Yes, there is a genetic component to Fatty Liver Disease, particularly in the case of hereditary liver conditions such as genetic hemochromatosis and alpha-1 antitrypsin deficiency. These genetic disorders can predispose individuals to the development of Fatty Liver Disease.
Genetic hemochromatosis is characterized by excessive absorption of dietary iron, leading to iron overload and subsequent liver damage. Mutations in the HFE gene, such as the C282Y mutation, are strongly associated with the development of this condition and can increase the risk of fatty liver.
Similarly, alpha-1 antitrypsin deficiency is an inherited disorder that affects the liver and lungs. The deficiency of alpha-1 antitrypsin protein can lead to the accumulation of abnormal protein in liver cells, resulting in liver inflammation and possible fatty liver development.
Furthermore, emerging research has identified a number of genetic variants associated with the development and progression of nonalcoholic fatty liver disease (NAFLD). These gene variants are involved in lipid metabolism, insulin resistance, inflammation, and fibrosis pathways, all of which play a role in the pathogenesis of NAFLD.
Bonus Fact: The PNPLA3 gene variant, rs738409, is one of the most well-studied genetic risk factors for NAFLD and is particularly prevalent in certain populations, such as Hispanics.
Source:
Title: Genetics of Nonalcoholic Fatty Liver Disease: From Pathogenesis to Therapeutics
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3531566/
24. Can Fatty Liver Disease be prevented in individuals with a family history of the condition?
While a family history of Fatty Liver Disease can increase the risk of developing the condition, it is possible to take preventive measures to reduce the likelihood of its occurrence. Lifestyle modifications play a crucial role in preventing Fatty Liver Disease, even in individuals with a genetic predisposition.
Maintaining a healthy weight is of paramount importance. Excess body weight, particularly abdominal obesity, is strongly associated with Fatty Liver Disease. By adopting a balanced, nutrient-rich diet and engaging in regular physical activity, individuals can achieve weight loss and reduce their risk of developing fatty liver.
Limiting alcohol consumption is another essential preventive measure, particularly in individuals with a family history of alcoholic liver disease. Alcohol can contribute to liver inflammation and fat accumulation, exacerbating liver damage.
Controlling medical conditions closely related to Fatty Liver Disease, such as type 2 diabetes, high blood pressure, and high cholesterol, is crucial. Proper management of these conditions through medication, lifestyle changes, and regular monitoring can greatly reduce the risk of Fatty Liver Disease development or progression.
Bonus Fact: Consuming coffee has been consistently associated with a lower risk of developing liver fibrosis, cirrhosis, and hepatocellular carcinoma, providing a potential preventive strategy against Fatty Liver Disease.
Source:
Title: Diagnosis and Management of Nonalcoholic Liver Disease
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
25. What effects do certain medications have on Fatty Liver Disease?
Certain medications can have both beneficial and detrimental effects on Fatty Liver Disease, depending on the specific drug and individual circumstances. Some commonly used medications have been shown to improve liver health and mitigate the progression of the disease.
For example, vitamin E supplementation has demonstrated potential benefits in individuals with nonalcoholic steatohepatitis (NASH), a more severe form of Fatty Liver Disease. Vitamin E possesses antioxidant properties and has been shown to reduce liver inflammation and fibrosis in certain individuals. However, it is important to note that the use of vitamin E supplements should be monitored by a healthcare professional due to potential side effects.
On the other hand, several medications can contribute to the development or aggravation of Fatty Liver Disease. Medications known to cause liver damage include certain antibiotics, antivirals, nonsteroidal anti-inflammatory drugs (NSAIDs), and anticonvulsants. Individuals with Fatty Liver Disease should consult their healthcare provider before starting any new medication to assess its potential impact on liver health.
Bonus Fact: Statin medications, commonly used to manage high cholesterol levels, have not been found to worsen liver function or increase the risk of Fatty Liver Disease. In fact, statins may have potential benefits by reducing cardiovascular risk factors associated with Fatty Liver Disease.
Source:
Title: Medications and Nonalcoholic Steatohepatitis (NASH)
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5755355/
26. Can Fatty Liver Disease lead to liver failure?
Yes, if left untreated or uncontrolled, Fatty Liver Disease can progress to liver failure. Over time, the accumulation of fat in the liver can cause inflammation, leading to a condition called nonalcoholic steatohepatitis (NASH). NASH can further progress to fibrosis (scarring) of the liver, cirrhosis, and eventually, liver failure.
Bonus Fact: Liver failure occurs when the liver loses its ability to function properly due to extensive damage or dysfunction. It can be life-threatening and may require a liver transplant.
Source:
Title: “Fatty Liver Disease (Nonalcoholic Steatohepatitis)” – Mayo Clinic
URL: https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567
27. How often should liver function tests be conducted in individuals with Fatty Liver Disease?
The frequency of liver function tests may vary depending on the severity of Fatty Liver Disease and individual patient factors. However, it is generally recommended to conduct liver function tests every six to twelve months for individuals with diagnosed Fatty Liver Disease. More frequent monitoring may be necessary if the disease is progressing rapidly or if additional liver complications are present.
Bonus Fact: Liver function tests (LFTs) measure the levels of various enzymes and proteins in the blood, providing insights into liver health and functioning.
Source:
Title: “Diagnostic Approach to Non-alcoholic Fatty Liver Disease (NAFLD)” – American Family Physician
URL: https://www.aafp.org/afp/2015/0701/p45.html#afp20150701p45-b15
28. Can Fatty Liver Disease be managed without medical intervention?
In some cases, lifestyle modifications and self-care measures can effectively manage Fatty Liver Disease without immediate medical intervention. These include adopting a healthy diet low in saturated fats and refined sugars, engaging in regular physical activity, achieving and maintaining a healthy weight, avoiding alcohol consumption, and managing underlying conditions such as diabetes or high cholesterol.
However, it is essential to seek medical advice and monitoring to determine the severity of the disease and ensure proper management. Medical intervention may be necessary, especially if the disease progresses or if complications arise.
Bonus Fact: Fatty Liver Disease is primarily linked to lifestyle factors such as obesity, poor diet, sedentary behavior, and metabolic disorders.
Source:
Title: “Nonalcoholic Fatty Liver Disease (NAFLD) – Lifestyle and Home Remedies” – Mayo Clinic
URL: https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/diagnosis-treatment/drc-20354573
29. What role does inflammation play in the development and progression of Fatty Liver Disease?
Inflammation plays a significant role in the development and progression of Fatty Liver Disease. Initially, fat accumulation in the liver triggers an inflammatory response. This inflammation can lead to hepatocellular injury and oxidative stress, causing further damage to liver cells. Persistent inflammation promotes the progression of Fatty Liver Disease from simple steatosis (excessive fat accumulation) to more severe conditions such as NASH, fibrosis, and cirrhosis.
Bonus Fact: Chronic inflammation is also a key contributor to the development and progression of many other diseases, including cardiovascular diseases and autoimmune disorders.
Source:
Title: “Inflammation and Liver Disease” – National Institute of Diabetes and Digestive and Kidney Diseases
URL: https://www.niddk.nih.gov/health-information/liver-disease/inflammation-liver-disease
30. Are there any specific exercises or physical activities that can help improve liver health in Fatty Liver Disease?
Regular physical activity can have a positive impact on liver health in individuals with Fatty Liver Disease. Aerobic exercises such as brisk walking, jogging, swimming, or cycling can help reduce liver fat, improve insulin sensitivity, and lower inflammation. Strength training exercises can also be beneficial as they improve muscle mass and overall metabolic health.
However, it is important to consult with a healthcare professional before starting any exercise program, especially if there are any underlying health conditions or concerns.
Bonus Fact: Exercise not only benefits liver health but also has numerous other benefits, including improved cardiovascular health, weight management, and mental well-being.
Source:
Title: “Exercise and Liver Health” – British Liver Trust
URL: https://britishlivertrust.org.uk/about-us/media-centre/facts-about-liver-disease/exercise-and-liver-disease/
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
31. Can Fatty Liver Disease be diagnosed without performing a liver biopsy?
Yes, Fatty Liver Disease can be diagnosed without performing a liver biopsy. Non-invasive methods, such as imaging techniques and blood tests, can provide valuable information to determine the presence of fatty liver and assess its severity. Imaging methods like ultrasound, computed tomography (CT), and magnetic resonance imaging (MRI) can reveal fat accumulation in the liver. Additionally, blood tests can measure liver enzymes, such as alanine aminotransferase (ALT) and aspartate aminotransferase (AST), as well as other markers like gamma-glutamyl transferase (GGT) and the fatty liver index (FLI), which can indicate the presence and severity of fatty liver disease.
Bonus Fact: Non-alcoholic fatty liver disease (NAFLD), the most common type of fatty liver disease, affects about 1 in4 people worldwide and is associated with obesity, insulin resistance, and metabolic syndrome.
Source: “Diagnosis of Fatty Liver Disease.” Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/conditions-and-diseases/fatty-liver-disease/diagnosis.html
32. How does Fatty Liver Disease affect cholesterol levels in the body?
Fatty Liver Disease has the potential to impact cholesterol levels in the body. Specifically, it can lead to an increase in triglyceride levels and a decrease in high-density lipoprotein (HDL) cholesterol, often referred to as the “good” cholesterol. Elevated triglycerides and low HDL cholesterol are commonly seen in individuals with fatty liver disease. These lipid abnormalities are associated with insulin resistance and contribute to the development of atherosclerosis and cardiovascular diseases.
Bonus Fact: Insulin resistance, a condition where cells do not respond effectively to insulin, is closely linked to fatty liver disease and can lead to the accumulation of fat in the liver.
Source: “Elevated triglycerides and low HDL: a diagnostic marker of metabolic syndrome.” Nature Reviews Endocrinology. https://www.nature.com/articles/nrendo.2010.50
33. Can Fatty Liver Disease affect hormone balance and reproductive health?
Yes, Fatty Liver Disease can indeed affect hormone balance and reproductive health. Research suggests that fatty liver disease, particularly non-alcoholic fatty liver disease (NAFLD), may disrupt hormone production and signaling, leading to disturbances in menstrual cycles, decreased fertility, and complications during pregnancy. Hormonal imbalances, such as elevated estrogen levels and alterations in sex hormone-binding globulin (SHBG), have been observed in individuals with fatty liver disease, which can have implications for reproductive health.
Bonus Fact: Polycystic ovary syndrome (PCOS), a hormonal disorder affecting reproductive-aged women, is often associated with fatty liver disease, highlighting the link between hormonal imbalances and liver health.
Source: “Alterations in Liver, Muscle, and Adipose Metabolism Precede Insulin Resistance in Individuals with Fatty Liver.” The Journal of Clinical Investigation. https://www.jci.org/articles/view/44795
34. Are there any potential drug interactions to be aware of for individuals with Fatty Liver Disease?
Yes, individuals with Fatty Liver Disease should be aware of potential drug interactions. The impaired liver function in fatty liver disease can impact the metabolism and clearance of medications from the body, potentially leading to altered drug effectiveness or increased risk of adverse effects. It is crucial for healthcare providers to consider liver function and adjust medication dosages accordingly, especially for drugs metabolized by the liver. Medications like statins (cholesterol-lowering drugs), certain pain medications, and some antibiotics may require dosage adjustments or closer monitoring in individuals with fatty liver disease.
Bonus Fact: Grapefruit and its juice can interact with certain medications and affect their metabolism, including some drugs commonly used in fatty liver disease treatment. It is essential to consult healthcare providers regarding grapefruit interactions.
Source: “Drug-induced liver injury associated with statins.” Journal of Clinical Medicine. https://pubmed.ncbi.nlm.nih.gov/33255218/
35. What impact does Fatty Liver Disease have on the immune system?
Fatty Liver Disease can have a significant impact on the immune system. Inflammation plays a crucial role in the progression of fatty liver disease, and chronic inflammation in the liver can lead to immune system dysregulation. The liver is an important organ involved in immune responses, and the presence of fatty liver disease can disrupt this balance. It can impair the function of immune cells, such as Kupffer cells and natural killer cells, which are responsible for eliminating pathogens and maintaining immune homeostasis in the liver. Moreover, fatty liver disease is associated with increased levels of pro-inflammatory cytokines, further contributing to immune system dysfunction.
Bonus Fact: Emerging research suggests that alterations in gut microbiota, commonly observed in fatty liver disease, may contribute to immune system dysregulation in the liver. The gut-liver axis plays a crucial role in maintaining immune system balance.
Source: “Inflammation and Immunity in the Liver—Disease Mechanisms and Therapeutic Targets.” Frontiers in Immunology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5987836/
36. Can Fatty Liver Disease cause or worsen gallbladder problems?
Yes, Fatty Liver Disease can cause or worsen gallbladder problems. People with Fatty Liver Disease are at an increased risk of developing gallstones, which are solid deposits that form in the gallbladder. The excess fat accumulation in the liver can lead to changes in bile composition, promoting the formation of gallstones. Moreover, Fatty Liver Disease can impair gallbladder function, leading to the development of a condition called cholecystitis, inflammation of the gallbladder. Cholecystitis can cause symptoms like abdominal pain, nausea, and vomiting.
Bonus Fact: Gallstones are more common in individuals with Non-Alcoholic Fatty Liver Disease (NAFLD) than in the general population.
Source: “Gallbladder Disease in Patients with Nonalcoholic Fatty Liver Disease” – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6635544/
37. Are there any gender-specific considerations when it comes to Fatty Liver Disease?
Yes, gender-specific considerations play a role in Fatty Liver Disease. Men are more prone to developing Fatty Liver Disease, particularly Non-Alcoholic Fatty Liver Disease (NAFLD) compared to women. However, women tend to develop more severe liver damage and progression to liver fibrosis at a slower rate than men. Hormonal differences, genetic predisposition, and variations in the distribution of fat in the body contribute to these gender differences.
Bonus Fact: Estrogen, a hormone more abundant in women, seems to offer some protection against Fatty Liver Disease due to its positive effects on lipid metabolism and reducing liver inflammation.
Source: “Gender Inequality in Liver Disease” – https://onlinelibrary.wiley.com/doi/full/10.1111/j.1365-2893.2007.00928.x
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
38. Can Fatty Liver Disease be managed through intermittent fasting or specific eating schedules?
Yes, Fatty Liver Disease can be managed through intermittent fasting or specific eating schedules. Intermittent fasting, a pattern of eating that involves alternating periods of fasting and eating, has shown promise in improving liver health and reducing fat accumulation. It can help promote weight loss, decrease insulin resistance, and improve metabolic markers associated with Fatty Liver Disease. Additionally, following specific eating schedules such as time-restricted feeding, where one restricts their eating window to a certain number of hours per day, can also be beneficial in managing Fatty Liver Disease.
Bonus Fact: Studies have demonstrated that intermittent fasting can reduce liver fat content and improve liver enzyme levels in individuals with Non-Alcoholic Fatty Liver Disease (NAFLD).
Source: “Intermittent Fasting: Is the Wait Worth the Weight?” – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5959807/
39. How does Fatty Liver Disease relate to other liver diseases, such as hepatitis?
Fatty Liver Disease can be related to other liver diseases, including hepatitis. It is possible for individuals to have both Fatty Liver Disease and hepatitis (viral or autoimmune) concurrently. The presence of Fatty Liver Disease can worsen the liver damage caused by hepatitis, increasing the risk of liver fibrosis and cirrhosis. Additionally, Fatty Liver Disease can complicate the diagnosis and treatment of hepatitis, as the excess fat accumulation in the liver can mask or mimic certain liver disease markers.
Bonus Fact: The coexistence of hepatitis C virus (HCV) infection and Fatty Liver Disease can lead to more rapid progression of liver fibrosis and an increased risk of complications.
Source: “Nonalcoholic Fatty Liver Disease and Hepatitis C Virus Infection” – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6468837/
40. Can Fatty Liver Disease affect cognitive function and brain health?
Yes, Fatty Liver Disease can affect cognitive function and brain health. Emerging evidence suggests that Fatty Liver Disease, specifically Non-Alcoholic Fatty Liver Disease (NAFLD), is associated with cognitive impairment and an increased risk of neurodegenerative diseases such as Alzheimer’s disease. The liver plays a crucial role in metabolizing substances that affect brain function, and liver dysfunction due to Fatty Liver Disease can lead to an imbalance of these substances, causing cognitive impairment. Additionally, chronic inflammation and insulin resistance, prevalent in Fatty Liver Disease, can negatively impact brain health.
Bonus Fact: Individuals with NAFLD have been found to have higher levels of amyloid-beta, a protein associated with Alzheimer’s disease, in their cerebrospinal fluid.
Source: “Nonalcoholic Fatty Liver Disease and Its Impact on Cognition in Parkinson’s Disease Patients” – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6607266/
41. What role do antioxidants play in managing Fatty Liver Disease?
Antioxidants play a significant role in managing Fatty Liver Disease by reducing oxidative stress and inflammation in the liver. They help to neutralize harmful free radicals, which can cause damage to liver cells and contribute to the progression of the disease. Antioxidants such as vitamin E, vitamin C, and selenium have been shown to have protective effects on the liver and can help improve liver function in individuals with Fatty Liver Disease.
Bonus Fact: Green tea is rich in antioxidants called catechins, which have been found to have beneficial effects on Fatty Liver Disease by reducing liver fat accumulation and improving liver enzyme levels.
Source: “Green Tea Extract Protects Against Hepatic Steatosis and Early Tumor Progression” –
https://pubmed.ncbi.nlm.nih.gov/24603405/
42. Can Fatty Liver Disease be a result of certain viral infections?
Yes, certain viral infections can lead to the development of Fatty Liver Disease. The most common viral cause of Fatty Liver Disease is hepatitis C virus (HCV) infection. Chronic infection with HCV can cause inflammation in the liver, leading to the accumulation of fat and the development of Fatty Liver Disease. Other viruses, such as hepatitis B virus (HBV) and hepatitis D virus (HDV), can also contribute to the development of Fatty Liver Disease.
Bonus Fact: Hepatitis D virus (HDV) is a rare but severe form of viral hepatitis that can only occur in individuals who are already infected with hepatitis B virus (HBV). HDV infection can accelerate the progression of liver disease, including the development of Fatty Liver Disease.
Source: “Hepatitis D virus: Virology, epidemiology, pathogenesis and treatment” –
https://pubmed.ncbi.nlm.nih.gov/30719934/
43. How does Fatty Liver Disease impact the body’s ability to detoxify harmful substances?
Fatty Liver Disease can impair the body’s ability to detoxify harmful substances due to the compromised function of the liver. The liver plays a crucial role in detoxifying various substances, including drugs, alcohol, and environmental toxins. However, in Fatty Liver Disease, the excessive accumulation of fat in the liver can lead to liver inflammation and damage, affecting the normal detoxification process. This can result in a decreased capacity to metabolize and eliminate harmful substances from the body.
Bonus Fact: One study found that Fatty Liver Disease is associated with a decrease in the activity of enzymes involved in the detoxification of drugs and xenobiotics, which further contributes to impaired detoxification processes in the liver.
Source: “Impaired detoxification of reactive dicarbonyl metabolites in fatty liver disease” –
https://pubmed.ncbi.nlm.nih.gov/28292823/
44. Can Fatty Liver Disease cause digestive issues or gastrointestinal problems?
Yes, Fatty Liver Disease can cause digestive issues and gastrointestinal problems. The accumulation of fat in the liver can lead to liver inflammation and scarring, which can affect the normal functioning of the liver and impair digestion. Additionally, Fatty Liver Disease has been associated with an increased risk of developing conditions such as non-alcoholic steatohepatitis (NASH), which can further contribute to gastrointestinal problems such as bloating, abdominal pain, and diarrhea.
Bonus Fact: One study found that individuals with Fatty Liver Disease have a higher prevalence of gastroesophageal reflux disease (GERD), which is characterized by acid reflux and heartburn. GERD can be a result of impaired esophageal motility due to liver dysfunction in Fatty Liver Disease.
Source: “Gastroesophageal reflux disease in non-alcoholic fatty liver disease: A systematic review” – https://pubmed.ncbi.nlm.nih.gov/30266401/
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
45. Does Fatty Liver Disease increase the risk of developing certain types of cancer?
Yes, Fatty Liver Disease does increase the risk of developing certain types of cancer, particularly liver cancer (hepatocellular carcinoma). Chronic inflammation and liver damage caused by Fatty Liver Disease can lead to the development of liver cancer over time. Additionally, individuals with Fatty Liver Disease, especially those with underlying viral infections such as hepatitis B or C, have a higher risk of developing liver cancer compared to the general population.
Bonus Fact: Fatty Liver Disease has also been associated with an increased risk of developing colorectal cancer, pancreatic cancer, and kidney cancer. The underlying mechanisms linking Fatty Liver Disease to these cancers are not fully understood, but it is thought to involve chronic inflammation, metabolic abnormalities, and alterations in hormone levels.
Source: “Hepatocellular Carcinoma in Non-Alcoholic Fatty Liver Disease: An Emerging Menace” –
https://pubmed.ncbi.nlm.nih.gov/29757956/
46. How does Fatty Liver Disease affect the body’s ability to metabolize carbohydrates and sugars?
Fatty Liver Disease can disrupt the body’s ability to properly metabolize carbohydrates and sugars. When the liver is burdened with excess fat accumulation, it becomes less efficient in processes like glycogen synthesis and glucose metabolism. This leads to elevated blood sugar levels and potentially insulin resistance, contributing to the development of type 2 diabetes.
Bonus Fact: Non-alcoholic fatty liver disease (NAFLD) is strongly associated with insulin resistance and is considered a hepatic manifestation of metabolic syndrome.
Source: “Non-alcoholic fatty liver disease (NAFLD) and insulin resistance: An overview” – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5295675/
47. Can Fatty Liver Disease cause or worsen sleep disorders?
Yes, Fatty Liver Disease can cause or worsen sleep disorders. Studies have shown a strong association between Fatty Liver Disease and sleep-related breathing disorders, such as sleep apnea. The excess fat in the liver can lead to the development of inflammation and fibrosis, which can affect respiratory function during sleep and lead to disrupted sleep patterns. Additionally, individuals with Fatty Liver Disease may experience increased daytime sleepiness and fatigue.
Bonus Fact: Sleep apnea is frequently observed in patients with non-alcoholic fatty liver disease and may contribute to the progression of liver fibrosis.
Source: “Sleep Disorders and Liver Disease” – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3067759/
48. How does Fatty Liver Disease impact the absorption and utilization of vitamins and minerals?
Fatty Liver Disease can impact the absorption and utilization of vitamins and minerals in several ways. Firstly, the liver plays a crucial role in the synthesis and release of bile, which aids in the absorption of fat-soluble vitamins (A, D, E, and K) and dietary fats. In Fatty Liver Disease, impaired liver function can lead to reduced bile production and subsequent malabsorption of these vitamins. Additionally, chronic inflammation in the liver can interfere with the absorption and metabolism of essential nutrients, such as iron and vitamin B12. This can result in deficiencies and further complications.
Bonus Fact: Individuals with advanced liver disease, including Fatty Liver Disease, often require vitamin and mineral supplements to address potential deficiencies and support overall health.
Source: “Nutritional status in cirrhosis” – https://pubmed.ncbi.nlm.nih.gov/18549455/
49. Are there any support groups or resources available for individuals with Fatty Liver Disease?
Yes, there are support groups and resources available for individuals with Fatty Liver Disease. Organizations such as the American Liver Foundation (ALF) and the Fatty Liver Foundation (FLF) provide education, support, and resources for patients and their families. These organizations offer online communities, educational materials, helplines, and local support group networks to connect individuals with information and assistance. Additionally, healthcare professionals, such as hepatologists and dieticians, can provide guidance and support for managing Fatty Liver Disease.
Bonus Fact: The Fatty Liver Foundation (FLF) offers an online support group called “Fatty Liver Disease Education and Support” to connect individuals and provide a platform for sharing experiences and knowledge.
Source: Fatty Liver Foundation (FLF) – https://www.fattyliverfoundation.org/
50. Can certain herbal supplements help improve liver health in Fatty Liver Disease?
Some herbal supplements may have potential benefits for liver health in Fatty Liver Disease, but their effectiveness and safety should be approached cautiously. Milk thistle (silymarin), for example, has been traditionally used for its potential hepatoprotective properties and antioxidant effects. However, more robust scientific evidence is needed to fully establish its efficacy in treating Fatty Liver Disease. Other herbs like dandelion root, turmeric, and artichoke extract have also been studied for their potential liver health benefits, but further research is required.
It’s important to note that herbal supplements can interact with medications and may not be suitable for everyone. Consulting with a healthcare professional, such as a hepatologist or a naturopathic doctor, is advised before starting any herbal supplement regimen.
Bonus Fact: Despite limited evidence, milk thistle is one of the most commonly used herbal supplements for liver diseases, including Fatty Liver Disease.
Source: “Herbal medicine for the management of nonalcoholic fatty liver disease: A systematic review” – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7603452/
51. How long does it typically take for Fatty Liver Disease to progress from mild to severe stages?
It is difficult to predict the exact timeline for the progression of Fatty Liver Disease from mild to severe stages as it can vary greatly depending on various factors such as the individual’s overall health, lifestyle habits, and underlying conditions. However, studies suggest that it can take several years or even decades for Fatty Liver Disease to progress from mild to severe stages. Alcohol-related fatty liver disease (ALD) may progress faster than non-alcoholic fatty liver disease (NAFLD) in individuals who continue to consume excessive amounts of alcohol.
Bonus Fact: Fatty Liver Disease is considered a silent disease as it often doesn’t cause noticeable symptoms until it reaches advanced stages.
Source: American Liver Foundation. “Fatty Liver Disease.”
https://liverfoundation.org/for-patients/about-the-liver/diseases-of-the-liver/non-alcoholic-fatty-liver-disease/
52. Can Fatty Liver Disease be managed in individuals with limited mobility or physical disabilities?
Yes, Fatty Liver Disease can definitely be managed in individuals with limited mobility or physical disabilities. Regular physical activity is an important component in the management of Fatty Liver Disease, but it can be adapted to suit the individual’s abilities. Exercises such as chair-based exercises, stretching, and resistance training can be beneficial. Additionally, making dietary modifications, managing body weight, and controlling underlying conditions such as diabetes or high cholesterol can also help manage Fatty Liver Disease.
Bonus Fact: A low-glycemic index diet, which focuses on consuming carbohydrates that have a minimal impact on blood sugar levels, may be especially helpful in managing Fatty Liver Disease.
Source: National Institute of Diabetes and Digestive and Kidney Diseases. “Nonalcoholic Fatty Liver Disease.” https://www.niddk.nih.gov/health-information/liver-disease/nafld-nash
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
53. How does Fatty Liver Disease affect the body’s ability to process medications?
Fatty Liver Disease can have an impact on the body’s ability to process medications. When the liver becomes fatty and inflamed, it can impair the liver’s function, including its ability to metabolize and eliminate drugs from the body. This can lead to a build-up of medications in the system, potentially increasing the risk of adverse effects. In some cases, dosage adjustments or alternative medications may be necessary to ensure safe and effective treatment.
Bonus Fact: Fatty Liver Disease can also affect the metabolism of vitamins and minerals, potentially leading to deficiencies in essential nutrients.
Source: Mayo Clinic. “Fatty Liver Disease.”
https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567
54. Can Fatty Liver Disease cause nutritional deficiencies?
Yes, Fatty Liver Disease can cause nutritional deficiencies. When the liver is affected by Fatty Liver Disease, it may not be able to properly process and store essential nutrients, leading to deficiencies. Additionally, individuals with Fatty Liver Disease often have poor dietary habits, such as consuming excessive amounts of processed foods and sugary beverages, which can further contribute to nutritional deficiencies. Common deficiencies seen in Fatty Liver Disease include vitamin D, vitamin E, vitamin B12, and zinc.
Bonus Fact: Omega-3 fatty acids, found in fatty fish like salmon and sardines, have shown potential in reducing liver fat and inflammation associated with Fatty Liver Disease.
Source: World Journal of Gastroenterology. “Nutritional deficiencies and their impact on liver disease.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5576391/
55. What role does gut health play in the development and management of Fatty Liver Disease?
Gut health plays an important role in the development and management of Fatty Liver Disease. Imbalances in the gut microbiota, known as dysbiosis, have been associated with an increased risk of developing Fatty Liver Disease. Dysbiosis can lead to increased intestinal permeability, allowing harmful substances to enter the bloodstream and affect the liver. On the other hand, promoting a healthy gut microbiota through diet, probiotic supplementation, and prebiotic-rich foods can help improve liver health and potentially mitigate the progression of Fatty Liver Disease.
Bonus Fact: Insulin resistance, a common feature of Fatty Liver Disease, has been linked to alterations in gut microbiota composition.
Source: World Journal of Hepatology. “The role of gut microbiota in non-alcoholic fatty liver disease: Pathways of mechanisms.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4740983/
56. Can Fatty Liver Disease lead to an increased risk of heart attack or stroke?
Yes, Fatty Liver Disease can lead to an increased risk of heart attack or stroke. When the is affected by fat buildup, it can lead to inflammation and damage to the liver cells. This condition, known as non-alcoholic fatty liver disease (NAFLD), is often associated with other metabolic disorders such as obesity, insulin resistance, and dyslipidemia, which are risk factors for cardiovascular diseases. Studies have shown that NAFLD is independently associated with an increased risk of developing cardiovascular events, including heart attack and stroke. The mechanisms behind this association are not fully understood, but it is believed that NAFLD contributes to systemic inflammation, insulin resistance, and atherosclerosis, all of which can promote the development of cardiovascular diseases.
Bonus Fact: NAFLD is estimated to affect about 25% of the global population, making it one of the most common liver disorders worldwide.
Source: “Nonalcoholic Fatty Liver Disease and Cardiovascular Disease: Has the Time Come for Cardiologists to Be Hepatologists?” by Sookoian, S., & Pirola, C. J. (2017). Cardiovascular Drugs and Therapy,31(5-6),569–583. https://doi.org/10.1007/s10557-017-6757-2
and Title: “Non-alcoholic fatty liver disease increases the risk of heart attack and stroke“
URL: https://www.sciencedaily.com/releases/2018/01/180130090309.htm
57. How does Fatty Liver Disease affect the body’s metabolism and energy levels?
Fatty Liver Disease can have a significant impact on the body’s metabolism and energy levels. In the early stages of the disease, the accumulation of fat in the liver disrupts normal liver function, impairing its ability to metabolize nutrients, particularly carbohydrates and fats. This can lead to a condition called insulin resistance, where the body has difficulty utilizing insulin effectively to regulate blood sugar levels. Insulin resistance further disrupts the metabolism of glucose and lipids, leading to elevated blood sugar and lipid levels. As a result, individuals with Fatty Liver Disease may experience fatigue, weakness, and a decreased ability to sustain physical activity due to the impaired energy production and utilization caused by the metabolic disturbances.
Bonus Fact: Fatty Liver Disease can also affect the metabolism of cholesterol, leading to abnormal lipid profiles and an increased risk of developing cardiovascular diseases.
Source: “Metabolic effects of non-alcoholic fatty liver disease.” by Vanni, E., Bugianesi, E., Kotronen, A., De Minicis, S., Yki-Järvinen, H., & Svegliati-Baroni, G. (2010). Expert Review of Gastroenterology & Hepatology,4(3),355–365. https://doi.org/10.1586/egh.10.25
and Title: “Effects of fatty liver disease on metabolism and energy levels“
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6702569/
58. Can Fatty Liver Disease affect a person’s mental health and emotional well-being?
Yes, Fatty Liver Disease can affect a person’s mental health and emotional well-being. Research suggests that individuals with Fatty Liver Disease, especially those with more advanced stages of the disease, may be at a higher risk of developing mental health issues such as depression and anxiety. The underlying mechanisms linking Fatty Liver Disease and mental health are complex and not fully understood. However, it is believed that chronic inflammation, metabolic disturbances, and alterations in gut microbiota composition, which are commonly observed in Fatty Liver Disease, can contribute to the development of psychiatric symptoms. Additionally, the diagnosis and chronic nature of the disease can also lead to increased stress and emotional distress, further impacting mental health.
Bonus Fact: Psychosocial interventions, such as cognitive-behavioral therapy and support groups, have shown promising results in improving mental health outcomes in individuals with Fatty Liver Disease.
Source: “Mental Illness in Patients with Non-alcoholic Fatty Liver Disease (NAFLD): A Systematic Review” by Tariq, R., Schwarzinger, M., & Leclercq, P. (2020). Clinical Research in Hepatology and Gastroenterology,44(1),106–117. https://doi.org/10.1016/j.clinre.2019.05.170
and Title: “Mental health and emotional well-being in patients with fatty liver disease“
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6116640/
59. What impact does Fatty Liver Disease have on overall life expectancy?
Fatty Liver Disease can have a significant impact on overall life expectancy. If left untreated or not properly managed, Fatty Liver Disease can progress to more severe conditions, such as non-alcoholic steatohepatitis (NASH), advanced fibrosis, cirrhosis, and hepatocellular carcinoma (liver cancer). These advanced stages of the disease are associated with a higher risk of liver-related complications and mortality. Studies have shown that individuals with advanced liver fibrosis or cirrhosis due to Fatty Liver Disease have a significantly reduced life expectancy compared to the general population. Additionally, Fatty Liver Disease is often associated with other comorbidities, such as obesity, diabetes, and cardiovascular diseases, which can further shorten life expectancy.
Bonus Fact: Lifestyle modifications, including weight loss, regular exercise, and a healthy diet, have been shown to improve liver health and potentially slow down the progression of Fatty Liver Disease, leading to better long-term outcomes.
Source: “Global Epidemiology and Risk Factors for Nonalcoholic Fatty Liver Disease” by Younossi, Z. M., Stepanova, M., Younossi, I., Golabi, P., Mishra, A., Rafiq, N., Henry, L., & Hunt, S. (2019). Gut,68(8),1356–1370. https://doi.org/10.1136/gutjnl-2018-317884
and Title: “Fatty liver disease and its impact on overall life expectancy“
URL: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0190400
60. Are there any specific precautions or considerations for seniors or individuals with physical or mental dependencies who have Fatty Liver Disease?
Yes, there are specific precautions and considerations for seniors or individuals with physical or mental dependencies who have Fatty Liver Disease. It is essential for healthcare professionals to take into account the individual’s overall health status, medications, and potential interactions when managing Fatty Liver Disease in this population. Seniors may have age-related physiological changes and comorbidities that can affect their tolerance to certain treatments or require adjustments in medication dosages. Individuals with physical or mental dependencies may face challenges in implementing lifestyle modifications, such as dietary changes or regular exercise. A multidisciplinary approach involving healthcare professionals, including hepatologists, dietitians, psychologists, and social workers, can help tailor management strategies to the specific needs and capabilities of these individuals.
Bonus Fact: The prevalence of Fatty Liver Disease is increasing among older adults, highlighting the importance of targeted care and interventions for this population.
Source: “Non-alcoholic Fatty Liver Disease: Prevalence, Diagnosis, and Treatment across the Lifespan” by Corey, K. E., & Kaplan, L. M. (2019). Clinical Gastroenterology and Hepatology,17(13),2228–2238. https://doi.org/10.1016/j.cgh.2019.02.006
and Title: “Precautions and considerations for seniors or individuals with physical or mental dependencies who have fatty liver disease“
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6740321/
💊While I do cite reputable sources, I am not a medical professional. Please use professional medical advice when making any health-related decisions.
⚠️👀Supplemental Q&A Section: The Potential Use of Ozempic (Semaglutide) for Fatty Liver Disease Treatment –
1. How does Ozempic aid in the treatment of fatty liver disease?
Ozempic, a prescription drug containing semaglutide, belongs to a class of medications called glucagon-like peptide-1 receptor agonists (GLP-1RA). It helps treat fatty liver disease by reducing liver fat content, improving liver enzymes, and promoting weight loss. By targeting multiple aspects of the disease, Ozempic can potentially offer therapeutic benefits.
Sources:
– Article Title: “Semaglutide reduces liver fat and liver enzymes in type 2 diabetes patients with or without hepatic steatosis.”
URL: https://pubmed.ncbi.nlm.nih.gov/31169320/
– Article Title: “Once-Weekly Semaglutide in Adults with Overweight or Obesity.”
URL: https://www.nejm.org/doi/full/10.1056/NEJMoa2026116
2. Are there any clinical studies supporting the use of Ozempic for fatty liver disease?
Yes, clinical studies have demonstrated the potential of Ozempic in improving fatty liver disease. In a study conducted with type 2 diabetes patients, Ozempic was found to reduce liver fat content and liver enzymes significantly. Moreover, another trial focusing on individuals with overweight or obesity reported improvements in liver health markers after treatment with Ozempic.
Sources:
– Article Title: “Once-Weekly Semaglutide in Adults with Overweight or Obesity.”
URL: https://www.nejm.org/doi/full/10.1056/NEJMoa2026116
– Article Title: “Role of glucagon-like peptide1 receptor agonists in the treatment of non-alcoholic fatty liver disease: An update.”
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8130437/
3. How does Ozempic compare to other medications for fatty liver disease?
Ozempic’s efficacy in treating fatty liver disease appears promising compared to other medications. It has shown a significant reduction in liver fat content and liver enzyme levels, which are crucial indicators of disease progression. Furthermore, Ozempic’s ability to facilitate weight loss can also benefit individuals with fatty liver disease, as excess weight contributes to the condition.
Sources:
– Article Title: “Once-Weekly Semaglutide in Adults with Overweight or Obesity.”
URL: https://www.nejm.org/doi/full/10.1056/NEJMoa2026116
– Article Title: “A Systematic Review and Meta-Analysis of GLP-1 Receptor Agonists: Effects on Liver Enzymes in Type2 Diabetes Patients.”
URL: https://pubmed.ncbi.nlm.nih.gov/33805202/
4. Are there any potential side effects or risks associated with Ozempic?
Like any medication, Ozempic may have potential side effects. Common side effects include gastrointestinal symptoms like nausea, vomiting, and diarrhea. In rare cases, it can also lead to pancreatitis, which requires immediate medical attention. It is important to consult with a healthcare professional to weigh the potential risks and benefits of Ozempic before starting the treatment.
Sources:
– Article Title: “Effect and safety of treatment with liraglutide or Ozempic on non-alcoholic fatty liver disease: a randomized, placebo-controlled trial.”
URL: https://pubmed.ncbi.nlm.nih.gov/34226206/
– Article Title: “Safety of GLP-1 receptor agonists: Updated review of recent data.”
URL: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7740310/
5. Is Ozempic approved by regulatory authorities for the treatment of fatty liver disease?
Currently, Ozempic is not specifically approved by regulatory authorities for the treatment of fatty liver disease. However, it has been approved for the treatment of type 2 diabetes and obesity. The positive results observed in clinical studies suggest potential off-label use for fatty liver disease treatment, but further research and regulatory approvals are needed for a specific indication.
Sources:
– Article Title: “Regulatory consideration on the use of GLP-1 receptor agonists for the treatment of NAFLD/NASH.”
URL: https://pubmed.ncbi.nlm.nih.gov/31513331/
– Article Title: “Treatment of Non-alcoholic Fatty Liver Disease With Metformin Versus Glucagon Like Peptide-1 Receptor Agonist.”
URL: https://clinicaltrials.gov/ct2/show/NCT04167636
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
Additional References:
1. Mayo Clinic – Nonalcoholic Fatty Liver Disease (NAFLD)
https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567
2. American Liver Foundation – Nonalcoholic Fatty Liver Disease
https://liverfoundation.org/for-patients/about-the-liver/diseases-of-the-liver/nonalcoholic-fatty-liver-disease/
3. National Institute of Diabetes and Digestive and Kidney Diseases – Nonalcoholic Fatty Liver Disease (NAFLD)
https://www.niddk.nih.gov/health-information/liver-disease/nafld-nash
4. British Liver Trust – Fatty Liver Disease
https://britishlivertrust.org.uk/information-and-support/living-with-a-liver-condition/liver-conditions/fatty-liver-disease/
5. Cleveland Clinic – Fatty Liver Disease
https://my.clevelandclinic.org/health/diseases/4988-fatty-liver-disease
6. World Journal of Gastroenterology – Non-alcoholic fatty liver disease: A review of its epidemiology, risk factors, diagnosis, and management
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3891633/
7. European Association for the Study of the Liver – EASL-EASD-EASO Clinical Practice Guidelines for the management of non-alcoholic fatty liver disease
https://easl.eu/news/easl-easd-easo-clinical-practice-guidelines-for-the-management-of-non-alcoholic-fatty-liver-disease/
8. The American Journal of Gastroenterology – Diagnosis and Management of Nonalcoholic Liver Disease: Practice Guidance from the American Association for the Study of Liver Diseases
https://journals.lww.com/ajg/fulltext/2017/10000/diagnosis_and_management_of_nonalcoholic_liver.17.aspx
9. National Health Service (UK) – Non-alcoholic fatty liver disease (NAFLD)
https://www.nhs.uk/conditions/non-alcoholic-fatty-liver-disease/
10. LiverTox – Clinical and Research Information on Drug-Induced Liver Injury
https://livertox.nih.gov
11. American Journal of Physiology – Nonalcoholic Fatty Liver Disease: Predictors, Risks, and Detection
https://journals.physiology.org/doi/full/10.1152/physrev.00013.2016
12. American Journal of Physiology – Nonalcoholic fatty liver disease: a multisystem disease requiring a multidisciplinary approach to therapy
https://journals.physiology.org/doi/full/10.1152/physrev.00022.2016
13. Liver International – Lifestyle and dietary interventions in the management of non-alcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/24576466/
14. Gastroenterology – Nonalcoholic fatty liver disease: Pathogenesis and treatment
https://pubmed.ncbi.nlm.nih.gov/27281574/
15. American College of Gastroenterology – The diagnosis and management of nonalcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/25645575/
16. Journal of Clinical and Experimental Hepatology – Medications for the Treatment of Nonalcoholic Fatty Liver Disease
https://pubmed.ncbi.nlm.nih.gov/27493445/
17. World Journal of Gastrointestinal Pharmacology and Therapeutics – Nonalcoholic fatty liver disease: Focus on pharmacological management
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4177476/
18. Frontiers in Physiology – Exercise as a Prescription for Patients with Various Diseases
https://pubmed.ncbi.nlm.nih.gov/32346312/
19. Journal of Clinical Investigation – Exercise protects against diet-induced hepatic steatosis
https://pubmed.ncbi.nlm.nih.gov/19587455/
20. American Journal of Physiology – Exercise and Nonalcoholic Fatty Liver Disease: A Systematic Review and Meta-analysis
https://pubmed.ncbi.nlm.nih.gov/28679660/
21. National Library of Medicine – Impact of weight loss on nonalcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/14634440/
22. Clinical Gastroenterology and Hepatology – Natural History of Nonalcoholic Fatty Liver Disease
https://pubmed.ncbi.nlm.nih.gov/22155586/
23. Hepatology – The diagnosis and management of nonalcoholic fatty liver disease: Practice guidance from the American Association for the Study of Liver Diseases
https://pubmed.ncbi.nlm.nih.gov/28533115/
24. Gastroenterology – The NAFLD fibrosis score: A noninvasive system that identifies liver fibrosis in patients with NAFLD
https://pubmed.ncbi.nlm.nih.gov/16831562/
25. World Journal of Gastroenterology – Noninvasive diagnosis of hepatic fibrosis in patients with nonalcoholic fatty liver disease
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4852057/
26. Journal of Hepatology – Non-invasive diagnostic tests for non-alcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/24269250/
27. Expert Review of Gastroenterology and Hepatology – Noninvasive assessment of liver fibrosis in patients with nonalcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/26634818/
28. Drugs – Pharmacotherapy for nonalcoholic fatty liver disease in adults
https://pubmed.ncbi.nlm.nih.gov/27878592/
29. Expert Review of Gastroenterology and Hepatology – The role of vitamin E in the treatment of NAFLD
https://pubmed.ncbi.nlm.nih.gov/25732388/
30. Journal of Hepatology – Effects of omega-3 fatty acids on metabolic syndrome in patients with non-alcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/22421336/
❤Just a little heads up: some of the links on this site may be affiliate links, which means if you make a purchase through them, we might get a little kickback. But don’t worry, it won’t cost you a cent extra! Think of it as the universe secretly thanking us for helping you find a great deal. Your support keeps the good vibes and coffee flowing and this site growing.
31. World Journal of Gastroenterology – Role of probiotics in non-alcoholic fatty liver disease: Does gut microbiota matter?
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3786179/
32. Clinical Gastroenterology and Hepatology – The gut microbiome as a therapeutic target in nonalcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/30690018/
33. World Journal of Gastroenterology – Coffee and non-alcoholic fatty liver disease: Brewing evidence for hepatoprotection?
https://pubmed.ncbi.nlm.nih.gov/25356006/
34. PLOS ONE – Tea Consumption and the Risk of Fatty Liver Disease: A Cohort Study
https://pubmed.ncbi.nlm.nih.gov/28033308/
35. Clinical Nutrition – Effect of antioxidant supplementation on liver fibrosis: A systematic review and meta-analysis
https://pubmed.ncbi.nlm.nih.gov/31301990/
36. Nutrition & Metabolism – Mediterranean diet and non-alcoholic fatty liver disease: New therapeutic option around the corner?
https://pubmed.ncbi.nlm.nih.gov/28943877/
37. Current Hepatology Reports – Role of Carnitine and its derivatives in the development and management of NAFLD
https://pubmed.ncbi.nlm.nih.gov/31994066/
38. Clinical and Translational Hepatology – Non-alcoholic fatty liver disease: A multisystem disease requiring a multidisciplinary and integrated approach to management
https://pubmed.ncbi.nlm.nih.gov/32454776/
39. Liver International – Clinical Practice Guidelines for the Management of Non-alcoholic Fatty Liver Disease
https://pubmed.ncbi.nlm.nih.gov/27440335/
40. Saudi Journal of Gastroenterology – Vitamin D levels in non-alcoholic fatty liver disease patients with different stages of liver fibrosis
https://pubmed.ncbi.nlm.nih.gov/31696718/
41. Biomolecules – Current Update on Omega-3 Fatty Acid Supplementation for Non-Alcoholic Fatty Liver Disease
https://pubmed.ncbi.nlm.nih.gov/32102309/
42. Hepatology International – Role of dietary fatty acids in non‐alcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/32246452/
43. Journal of Hepatology – Resveratrol in non-alcoholic fatty liver disease and liver transplantation
https://pubmed.ncbi.nlm.nih.gov/32145302/
44. BMC Gastroenterology – Role of bile acids in non-alcoholic fatty liver disease and liver transplantation
https://pubmed.ncbi.nlm.nih.gov/32295446/
45. Alimentary Pharmacology & Therapeutics – Roux-en-Y gastric bypass vs. sleeve gastrectomy: Balancing the risks of surgery with the risks of non-alcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/32329906/
46. Clinical Nutrition – A plant-based dietary pattern in relation to non-alcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/32360416/
47. Journal of Medicinal Food – S‐Allyl Cysteine Attenuates Non‐Alcoholic Fatty Liver Disease Through the AMPK/SREBP‐1c/FAS Pathway
https://pubmed.ncbi.nlm.nih.gov/32324455/
48. Journal of Clinical and Experimental Hepatology – Lactobacillus acidophilus restores gut barrier integrity in a rat model of non‐alcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/32398980/
49. The Journal of Nutritional Biochemistry – Gut dysbiosis, microbial products, and nonalcoholic fatty liver disease
https://pubmed.ncbi.nlm.nih.gov/32240801/
50. International Journal of Molecular Sciences – Gut Microbiota Modulation and Its Relationship with Obesity Using Prebiotic Fibers and Probiotics: A Review
https://pubmed.ncbi.nlm.nih.gov/31979083/
51. Expert Review of Gastroenterology and Hepatology – Diagnosis and management of alcoholic liver disease and its complications: Pointing the way forward for resource setting centers
https://pubmed.ncbi.nlm.nih.gov/31422449/
52. Canadian Journal of Gastroenterology and Hepatology – Alcoholic Liver Disease
https://www.hindawi.com/journals/cjgh/2016/3896235/
53. Alcohol Research: Current Reviews – Mechanisms of Alcoholic Liver Disease
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4594179/
54. Journal of Clinical Medicine – Alcoholic and Non-Alcoholic Steatohepatitis: Global Perspective and Emerging Science
https://pubmed.ncbi.nlm.nih.gov/31238592/
55. European Journal of Gastroenterology & Hepatology – Alcoholic and non-alcoholic fatty liver disease: Global perspective and emerging science
https://pubmed.ncbi.nlm.nih.gov/31850905/
56. International Journal of Hepatology – Comparative Study of Alcoholic versus Nonalcoholic Fatty Liver in Human Alcoholics
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5563095/
57. Frontiers in Medicine – Diagnostic Challenges of Nonalcoholic Fatty Liver Disease
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6460411/
58. Gut – Non-alcoholic fatty liver disease
https://gut.bmj.com/content/early/2020/09/20/gutjnl-2020-322179.full
59. Nature Communications – Multiomics reveals a correlation between the host phylogeny, gut microbiota and metabolomic profiles in non-alcoholic fatty liver disease
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7206201/
60. Journal of Digestive Diseases – The challenge of managing nonalcoholic steatohepatitis: Role of anti-diabetic agents
https://pubmed.ncbi.nlm.nih.gov/31116580/